Vaccine supply a sticking point for GP jabs
Computer booking glitches, overloaded call systems and supply uncertainty continue to hinder the COVID-19 vaccine rollout in South Australian clinics, although GPs say they’re encouraged by the number of people coming forward to receive their jab.

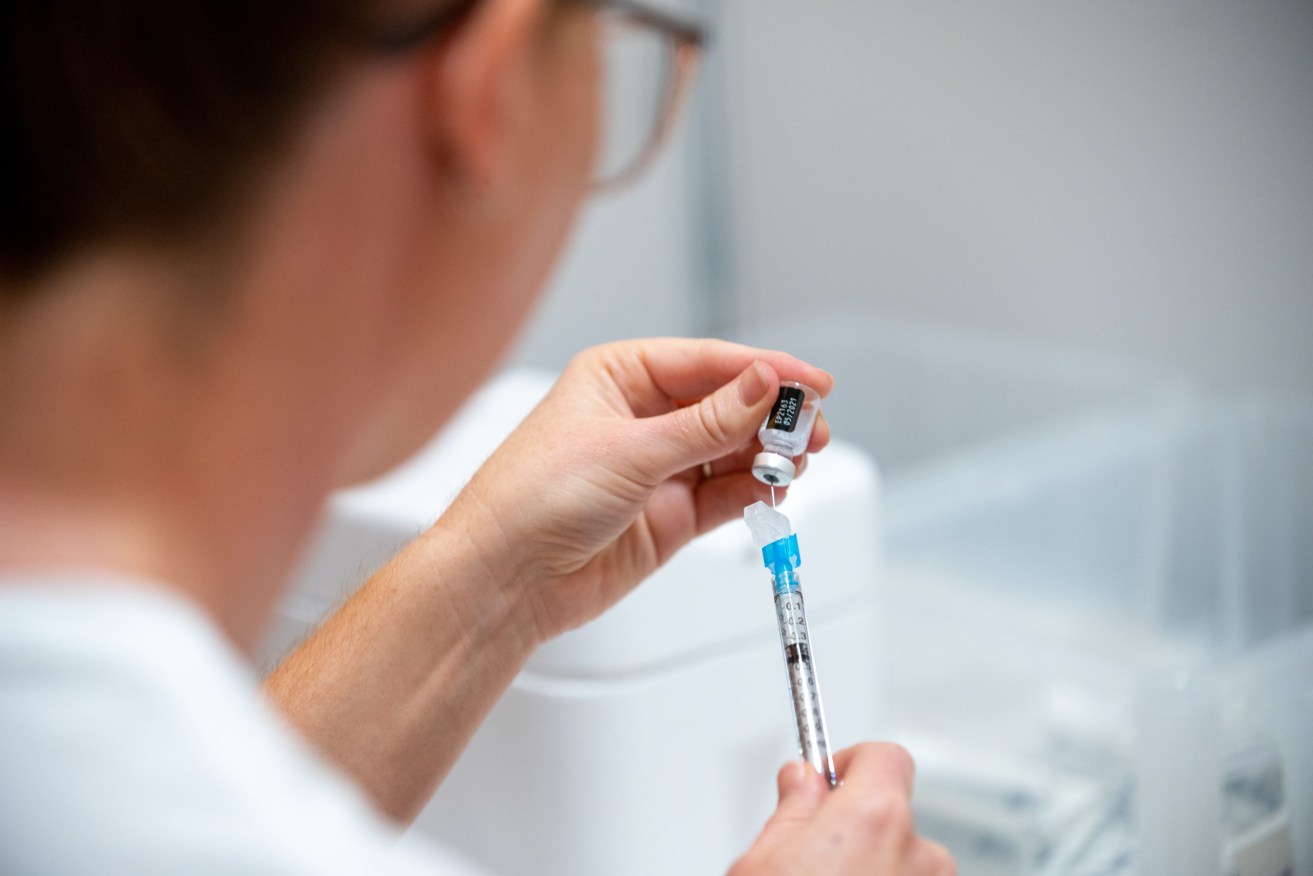
Photo: AAP/Josh Fernandes
The federal government’s COVID-19 vaccine rollout on Monday opened to all Australians between 50 and 69 years old, with state and territory clinics and some general practices now administering the AstraZeneca jab to the new demographic.
The latest stage of the rollout, phase 2a, extends to all participating GPs on May 17, following a national cabinet decision to adjust the vaccine rollout due to health advice recommending against using the AstraZeneca vaccine for under 50s due to very rare but sometimes fatal blood clots.
The majority of GPs only stock the AstraZeneca vaccine.
Adelaide GP Dr Alvin Chua, who works across clinics in Campbelltown and Newton, said his clinics were still struggling with call overloads from concerned patients.
“The booking website had glitches [on Monday] as the online platform had not accounted for those aged 50-70 being able to be booked in GP clinics such as ours,” Chua said.
“It wasn’t till after 2pm till the issue was fixed.
“Meanwhile our phone lines [on Monday] were inundated yet again, but having said that, I’m glad people are making enquiries and booking in to get immunised.”
A total of 172,408 vaccines have been administered in South Australia as of Tuesday, the majority of which have been administered by GPs and primary care centres (92,867 doses), followed by state-run clinics (62,094) and Commonwealth aged care centres (17,447).
Health at Campbelltown’s website currently asks patients not to call reception for vaccine related enquiries, as “the large volume of calls is impacting the ability of reception staff to attend to regular needs of our patients”.
Chua – who threatened to withdraw from the vaccine rollout last month after his clinic was “inundated” with angry callers concerned about receiving the AstraZeneca vaccine – said the government’s online booking system has been “good to minimise interaction with abusive callers”.
He said the “key issue is hesitancy and patient expectation”, and pointed to the problem of under 50s who have a chronic disease asking GPs to administer the Pfizer vaccine.
“[It’s] a common question that crops up and all we can do is suggest they contact the government-funded hospital co-located clinics,” Chua said.
“[The younger cohort] all want to wait for Pfizer but don’t realise that it may be months before new supplies arrive.”
Chua’s clinics are receiving a “steady” supply of 400 doses a week from the Commonwealth, but added “there are lots of GP clinics that have requested more vaccines for their patients but only getting as few as 50 doses a week”.
Adelaide GP Dr Rod Pearce, principal of four clinics across South Australia, is among those only receiving 50 doses a week from the federal government.
He says he has been stuck in a “circular argument” with patients who are unable to receive immediate information about when they can book in for a COVID-19 vaccination.
“That’s why it’s been so frustrating because you can’t plan … you can’t talk to people,” Pearce said.
He said his clinics would need 1000 backup doses to start vaccinating at a consistent rate.
“Then we will then start planning for routine and regular clinics on the basis that we’ll actually have enough vaccines to work with people,” he said.
“But we can’t start any of those conversations until we’ve got some [patients], and we can’t get some until we’ve got more than 50 [doses] a week because, really, that’s not any.”
Pearce’s concerns appear to be shared by GPs across the country.
The Australian General Practice Alliance, a national peak body for clinic owners, this morning said interim results from a survey of 38 member clinics reveals just one is administering COVID-19 vaccines at full capacity.
The remaining 37 said supply issues were limiting their ability to ramp up their vaccination program.
Chief Public Health Officer Nicola Spurrier on Monday said South Australia is aiming to vaccinate 80 per cent of the population by October, but this would depend on receiving an adequate supply of vaccine doses from the Commonwealth.
Dr Zakaria Baig, SA branch chair of the Royal Australian College of General Practices, said GPs have welcomed the move to expand the AstraZeneca rollout to over 50s, but an increase in dose supply is needed to support the rollout.
“What the GPs are saying is ‘yep Australia you’re asking us to do a lot more vaccinations, that’s fine, but you actually haven’t supplied us with more vaccines,” Baig said.
Baig is the principal of a Salisbury clinic which receives 100 doses a week from the Commonwealth, but he noted that “there are clinics larger than us still receiving 50 a week”.
He said the incorporation of the COVID vaccine program has added an extra 50 to 70 patients to his clinic’s weekly caseload.
“It has affected us quite a bit in terms of workforce … it ties up your front desk staff just wanting to deal with the patient because there are quite a large number of patients,” he said.
“So that’s been the biggest task for staff and people on the front desk, we still have to provide people service for the other non-vaccine related topics.
“And what we’re finding is that we’re sort of running out of appointments … because the focus is on the COVID delivery.”
Dr Rod Pearce called on the federal government to make the Medicare rebate for COVID-19 vaccine consultation equivalent to a standard consultation rather than a five-minute consultation.
“By the time you get nurses, by the time you get the consent, by the time you get the doctors, by the time you had the conversation – the five minutes consultation is in the books,” he said.
“It just feels like GPs are expected to pick up the tab rather than them being supported.”
On the issue of vaccine hesitancy, Pearce noted several requests from over 50s to receive the Pfizer vaccine instead of the AstraZeneca, but said these were “kind of an exception to the rule”.
“I tell them now that we’ve got a diagnosis, we’ve got a test, and we can treat [the clots] just like a fit of anaphylaxis,” he said.
“So [we] try to have that sort of conversation to say ‘there’s more risk but we can do something about it, we’re not just helpless or just waiting for a catastrophe’.”
Baig said consulting with patients on the AstraZeneca vaccine and “[dispelling] some of the myths they have” has been effective in reassuring patients in the jab’s safety.
“What we find is, particularly in a number of clinics, that some patients are not sure when we raise this issue,” he said.
“But after 10 minutes of consultation and discussion, we’re finding they change their mind and they say ‘yeah okay I’ll have it’.
“My message for those over 50s is to get vaccinated at the first opportunity, because we need as many people to come forward to be vaccinated as possible to protect the community.”
South Australia recorded one new COVID-19 cases on Wednesday from an overseas traveller in a medi-hotel. SA Health says they are monitoring the situation in NSW where there has been one new local coronavirus case, and will provide a list of exposure sites on their website shortly.
SA Police Commissioner Grant Stevens this morning said while he understands the “complex challenges” associated with the vaccine rollout, he is eager for the pace to pick up so authorities can remove more COVID-19 restrictions.
“The frustration for me is: the sooner we get that … critical mass vaccinated, the more opportunities we have to remove these restrictions,” Stevens told ABC Radio.
“But I’d also point out that right at this point in time I think South Australia is probably the most relaxed place in Australia when it comes to restrictions.”




