Dodging the double whammy of coronavirus and flu season
The coronavirus threat has risen as we head into flu season. Here’s a few things we can do to lessen our risk, writes C Raina MacIntryre.
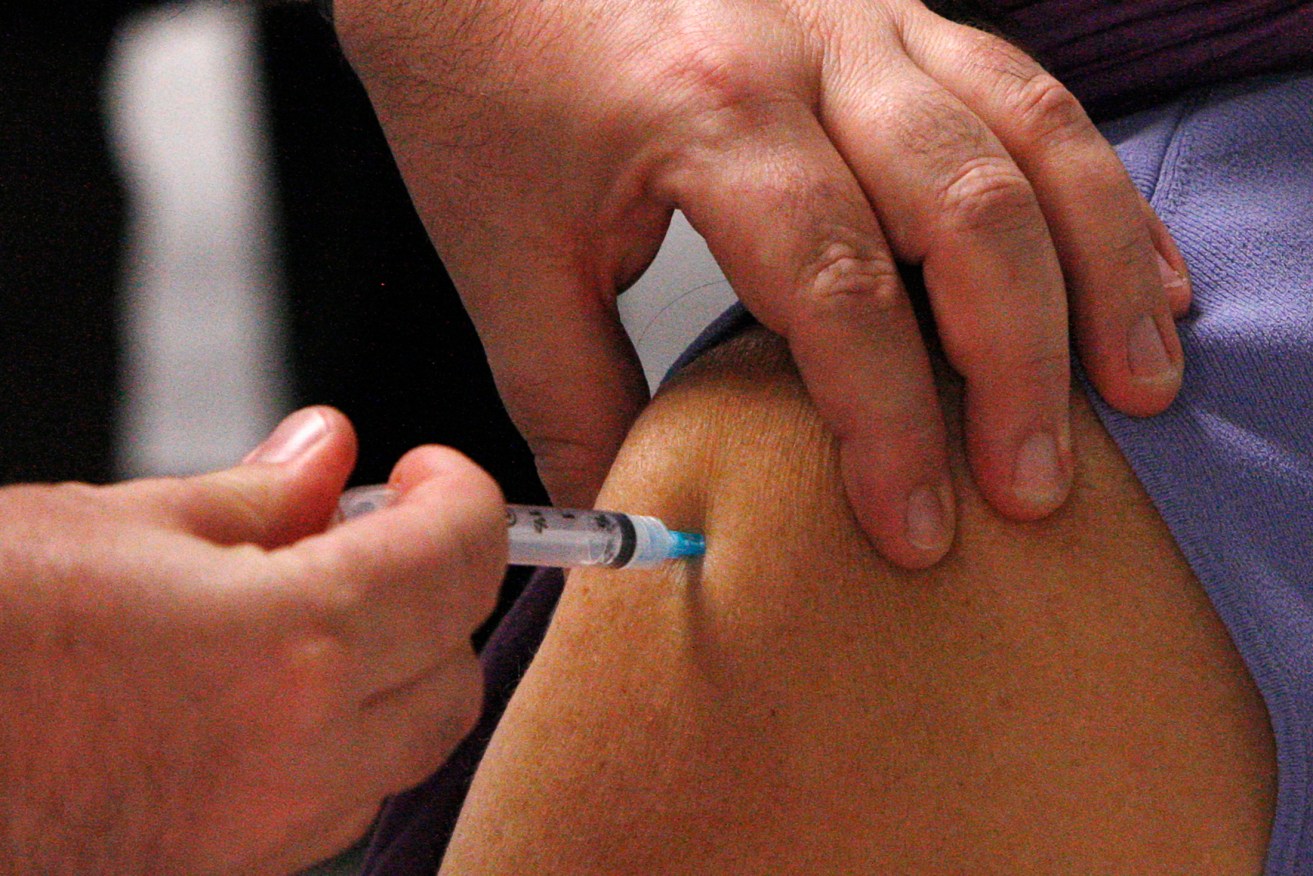
Photo: supplied
The prime minister yesterday announced that from May 1, people need to be vaccinated against the flu before visiting an aged care facility.
The idea is to limit the risk of the “dreaded duo” of respiratory diseases – influenza and coronavirus – affecting the frail and elderly.
We’re concerned about the combined impact of the flu and the coronavirus on us and our health system.
But we can minimise that impact.
Coronavirus peak set for flu season
The peak of COVID-19 cases in Australia is yet to come, with estimates numbers will double about every three to six days.
This exponential rise means Australia’s peak in COVID-19 cases may converge with our annual influenza season, which peaks on average in August each year.
Both influenza and coronavirus can cause severe illness, but the coronavirus is about ten times more deadly than the flu.
Both viruses cause severe pneumonia, so getting them together could be a serious blow to the lungs.
Severe infection with either virus can result in pneumonia and respiratory failure requiring mechanical ventilation, or even ECMO, a method of oxygenating the blood outside the body.
Infection with either virus affects older people and people with chronic diseases more severely, which makes these the highest risk groups for being infected with both viruses at once. People in aged care facilities are particularly at risk.
Influenza can severely affect infants and children under five years old.
We do not have as much information about COVID-19 in children, which may cause mild or no symptoms.
But a new study suggests it can be severe in 6% of kids, especially those under five years. A 14-year-old child in China has also died.
Co-infection with influenza has been documented in China. In one study, 34% of over 8,000 fever patients who were tested had COVID-19, and less than 1% were infected with COVID-19 and another virus, including influenza.
Health systems will be under more strain
Another impact of influenza and COVID-19 circulating simultaneously is on our health systems.
Every winter, we need to have extra hospital beds and staff to cope with influenza. However, for COVID-19, we will need to plan for more, as death rates, hospitalisation rates and ICU admission rates are higher.
So a severe epidemic of COVID-19 during our influenza season could result in a severely overloaded health system unable to cope, as we are seeing in Italy.
What can we do? Get the flu vaccine
We do not have a vaccine for COVID-19 yet, but we do have vaccines to protect against influenza.
So, if you’re at increased risk for influenza complications, make sure you’re vaccinated.
Influenza vaccination is recommended and funded in Australia for risk groups, such as people aged 65 years and over, people with chronic conditions such as heart, lung or neurological diseases, pregnant women, and for children six months to under five years old.
Flu vaccine is also recommended, but not funded, for people aged five to 65 years. Carers of vulnerable people, and people who work in health care, childcare or aged care should also get vaccinated.
Now that influenza vaccination is already available this season in pharmacies, it’s fast and convenient for busy working people to get vaccinated.
People at risk can be vaccinated any time from March to May. There is some evidence that flu vaccine immunity does not last a full 12 months, but timing of vaccination makes only a small difference to preventing influenza.
So if you forget to get the flu vaccine, it is still worth getting vaccinated any time later in the year.
What else can we do?
Both influenza and COVID-19 can be transmitted before symptoms occur or by people with no symptoms.
So to reduce the risk of transmission of either virus, the World Health Organisation recommends washing your hands frequently, coughing into your elbow, and cleaning and disinfecting frequently touched objects.
Indian cricket legend Sachin Tendulkar shows how to wash you hands properly.
Social distancing – such as maintaining spatial separation from other people, avoiding crowds, working from home – will also reduce the risk of both infections.
The more of these measures we use, combined with isolating sick people and quarantining their contacts, the more we can flatten the curve, to reduce the impact of both infectious diseases on individuals and the health system.
Older people and people with chronic diseases especially need to practice social distancing, and avoid unnecessary contact and travel.
We may even need to screen visitors to the home and ask them not to come if ill, especially if there are people at risk in the household.
Younger people, especially those living with older people, should be mindful of avoiding crowds and bringing infection into the household.
Aged care facilities will need to restrict visitors, as recommended in the latest health advice.
With winter almost upon us, we must use all these measures to reduce the combined impact of COVID-19 and influenza.
C Raina MacIntyre, Professor of Global Biosecurity, NHMRC Principal Research Fellow, Head, Biosecurity Program, Kirby Institute, UNSW
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Want to comment?
Send us an email, making it clear which story you’re commenting on and including your full name (required for publication) and phone number (only for verification purposes). Please put “Reader views” in the subject.
We’ll publish the best comments in a regular “Reader Views” post. Your comments can be brief, or we can accept up to 350 words, or thereabouts.
![]()





